Epilepsy Overview
Epilepsy is disorders characterized by recurrent unprovoked seizures due to abnormal & excessive electrical activity in the brain. Every episodic disorder is not a seizure and every seizure is not epilepsy. Diagnosis of epilepsy is often made by pediatric neurologist by thorough clinical evaluation supported by EEG & sometimes MRI.
Epilepsy means a tendency to have recurrent seizures.
Epilepsy leads to tremendous anxiety in the parents and witnessing the event leads to fear. Appropriate diagnosis & treatment, most children can be cured. The first step is correct diagnosis to be followed by starting the right medications.
Seizure Mimics (Non-Epileptic Attack Disorders- NEADs)
In newborn period, infancy, early or late childhood many conditions can mimic seizures. These conditions may be benign and need differentiation from seizures, thus avoiding unnecessary use of antiepileptic drugs and parental anxiety.

Single Seizure or first unprovoked seizure
Seizure is caused by abnormal and excessive electrical activity in the brain. Seizures which occurs without any provoking condition like fever is known as unprovoked seizure. The seizure may be epileptic. Epilepsy is a condition characterized by recurrent unprovoked seizures.
In children risk of recurrence is approximately 50%. Even a single seizure needs evaluation by experts like pediatric neurologist and Electroencephalogram (EEG) to understand the cause, risk of recurrence and need for medication.
Benign Epilepsies
Epilepsy is a condition characterized by recurrent unprovoked seizures. Benign epilepsies are common in children. There are different types of benign epilepsies which can be classified and diagnosed by pediatric eurologist with help of history, EEG and sometimes an MRI. They may or may not need medications.
Refractory Epilepsies
Seizures which do not get controlled with 2 or more well-chosen antiepileptic medications given regularly, under medical guidance in optimum doses for 6 months or more, are known as refractory seizures. Refractory seizures or refractory epilepsy needs detailed review and investigation to find the cause.
Epileptic Encephalopathies
Epileptic Encephalopathies are difficult epilepsies where the seizures are difficult to control, the child’s development, behavior, learning and sometimes alertness is affected. They may be genetic, metabolic or symptomatic. Epileptic Encephalopathies are serious disorders of brain and need extensive evaluation and aggressive treatment.
What is EEG (Electro Encephalo Graphy)?
This is most commonly ordered investigation. It records electrical activity in the brain. Abnormal electrical activity can be recorded in 40-50% children with epilepsy. 4% of normal children may also abnormal electrical activity. Therefore, EEG needs to be interpreted carefully with clinical correlation. Also interpreting pediatric EEGs needs certain amount of expertise and training and therefore better reported by a pediatric neurologist.
EEG recording – Preparation for EEG – instructions for parents
Hair should be washed & clean & off any oil before EEG.
- A sleep EEG gives better yield (natural sleep is preferred), therefore the child should be sleep withdrawn previous night with 4-5 hours of night sleep only. Do not allow sleep during the travel to EEG lab.
- Encourage a proper meal before the tests (Anesthesia is not used ever).
What is Video EEG?
This test is needed in some cases where it is important to determine nature of the event for diagnosis. Here we record EEG along with video of the child.
When is MRI needed?
This test is needed to see the structure of the brain to check for structural malformations, metabolic deposits or sometimes functional disorder.
MRI is not routinely needed in all children, but ordered to find the cause.
When to order Genetic & Metabolic Tests?
Some children have associated developmental delays, dysmorphism, and some children do not respond to regular treatment. It is important to further investigate these children for underlying genetic disorders as treatment may change in them.
Why did my child get a seizure?
Epilepsy may occur due to an inherited genetic tendency or a mutation. A structural change in the brain (sometimes called ‘symptomatic’) or damage caused by a brain injury at the time of birth, infections like meningitis can also lead to seizures.
Epilepsy Treatment
Emergency Treatment & First Aid What steps should I take when my child has a seizure?
- Be calm as most seizures are self-terminating.
- Keep the child in lateral position, protect him from injury- remove any harmful objects that the child may hit, cushion their head and loosen any tight clothing. Stay with the person until recovery is complete.
- Do not put anything in the mouth OR give anything to eat and drink until fully recovered.
- If seizure continues beyond 2 minutes, use Midazolam spray for nasal or buccal use in doses advised by your doctor.
- Hospitalize the child if seizures continue even after use of spray or he does not become conscious.
- Every seizure does not need hospitalization.
My child gets a seizure only with fever, what should I do?
Febrile seizures are harmless. If child gets a seizure, bring down the temperature with sponging using tap water. Manage the fever with paracetamol in adequate doses round the clock.
Does my child need long term medication?
Once epilepsy is diagnosed, we identify the right medication, which must be given for a period of 2 years of seizure freedom. Seizure recurrence needs a follow up visit for review.
Why Regular Follow Up?
Parents need regular follow up to report seizures to doctor and to review his behavior & school performance. Reporting of side effects if any is compulsory. Medicine should be stopped gradually after seizures freedom only after consulting the treating doctor.
Does my child need any modification of lifestyle? Epilepsy does not need any major change in lifestyle.
The child should continue his routine as earlier. Do not overprotect. Realistic expectations in behavior, academics and other life goals should be maintained. Anxious discussions can lead to low self-esteem and related complications like anxiety & poor academic performance. Switching to healthy dietary options, regular sleep, exercise help, but no specific dietary changes are required in most cases of routine/benign epilepsies.
What should be avoided?
Unsupervised swimming is to be avoided, as seizure while swimming can lead to drowning. Strobe lights in discotheques can precipitate a seizure and may be avoided.
Diets for Epilepsy
When to Use? Which diets can be advised?
We prefer modified Atkins diet, as it convenient, easy & effective.
Children whose seizures remain uncontrolled despite judicious use of medications are considered to have refractory epilepsy. We review the child for compliance, alternative diagnosis & offers dietary treatment options to drugs.
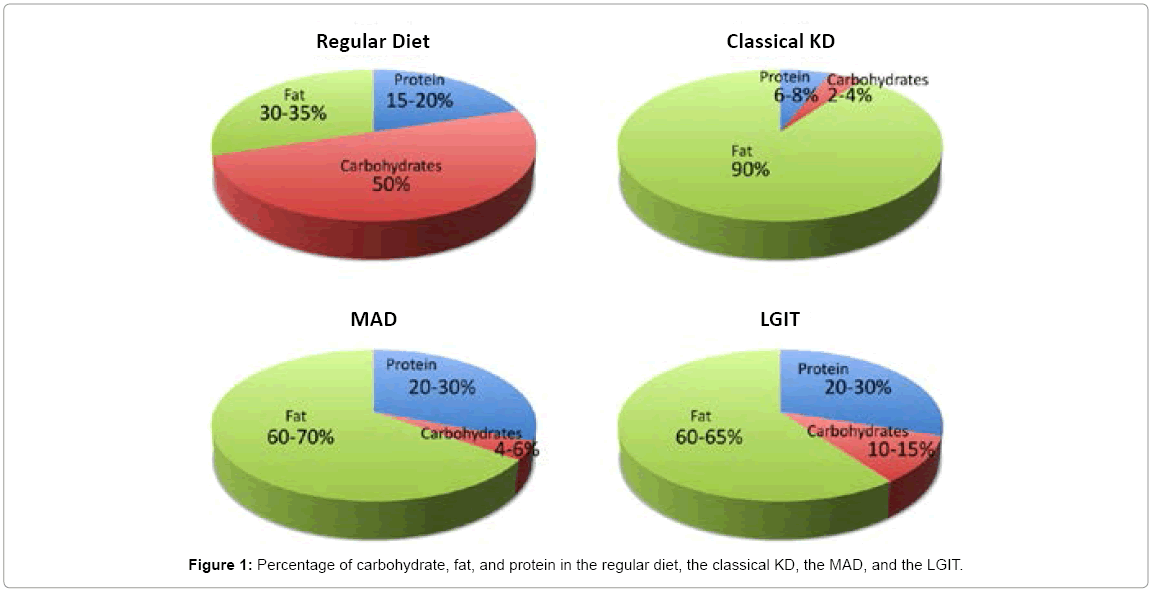
A. Modified Atkins diet(MAD)
A. MAD version is less complicated. Patients do not need admission to the hospital, no fasting or dietician is required to plan meals. MAD is more “user friendly” version of the diet & can be recommended for older children, teenagers and adults. It is simpler to follow, less limiting socially, and more palatable.
B. Ketogenic diet (KD)
B. KD is the oldest diet, it is complex and time-consuming & needs direction from a trained dietician and physician. The child may need hospitalization for fasting, and the parents are trained to weigh, measure and prepare foods. Calories & fluids are restricted, and foods are calculated in exact amounts. The ketogenic diet includes 80% fat, 15% protein, and 5% carbohydrate; the ratio of fat to carbohydrate plus protein ranges from 2:1 to 4:1, with higher ratios seen as more restrictive but more effective.
C. Low Glycemic Index diet (LGIT)
C. LGIT recommends ingestion of foods such as fruits, vegetables, nuts, and whole grains yields a slow, steady rise in serum glucose as compared with ingestion of refined grains. It recommends 40–60 g of carbohydrates with glycemic indices < 50 and 60% of energy from fat and 20–30% from protein.
D. The Medium-chain Triglyceride diet –
D. This is a variant of KD which uses medium-chain fatty acids provided in oil form (MCT oil) as a dietary supplement.

